Articles

Mindfulness, Mindful Breathing and Mast Cells
This guide explains the benefits of Mindfulness and breathwork and provides short exercises to try.

Lotus Flower Breathing
Lotus Flower Breathing is a gentle breathing exercise that helps to calm the nervous system and reduce stress. With thanks to Deborah Bircham from Live Well With Chronic Illness.

Hand Breathing
This simple breathing exercise has been provided to us by Deborah Bircham from Live Well With Chronic Illness.

Parent Carer Service Support Leaflet
This leaflet details the free service delivered by trained volunteers who can provide peer support to parents and carers who need it.

Peer Support Service Leaflet
This leaflet details the free service delivered by trained volunteers who can provide peer support to those who need it.
The international EAACI/GA²LEN/EuroGuiDerm/APAAACI guideline for the definition, classification, diagnosis, and management of urticaria
Zuberbier T, Abdul Latiff AH, Abuzakouk M, et al. The international EAACI/GA²LEN/EuroGuiDerm/APAAACI guideline for the definition, classification, diagnosis, and management of urticaria. Allergy. 2022;77:734–766. doi:10.1111/all.15090

Travelling with MCAS
This downloadable booklet contains tips and resources for managing Mast Cell Activation Disorders on the go, wherever you go.

Lesson Planning Questions for MCAS Considerations
This list can help teachers and other educators to include students living with MCAS, when planning lessons and classroom activities

Supporting Safe Learning for Students with MCAS Full Pack
This full resource pack is designed to help you share vital information about mast cell disorder with schools.

Supporting Safe Learning for Students with MCAS for Teachers
This resource has been designed to explain Mast Cell Activation Syndrome to Teachers and guide them in creating a safe environment for pupils.

Supporting Safe Learning for Students with MCAS
This kit has been specially designed for parents and primary caregivers of secondary school students who have a mast cell disorder, such as Mast Cell Activation Syndrome (MCAS).

Knowing our values
Knowing our values is important to help us to achieve fulfilment. Use this guide to help you plan what you need to be doing in order to feel a sense of purpose and fulfilment.

Life Audit
Are you meeting your Core Needs? Conducting a life audit can be an insightful exercise to help you evaluate and enhance your overall wellbeing.

Life Audit
Are you meeting your Core Needs? Conducting a life audit can be an insightful exercise to help you evaluate and enhance your overall wellbeing.
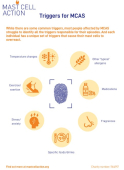
Triggers
This resource details some of the more common triggers of Mast Cell Activation Syndrome.

Symptoms of MCAS
This resource details some of the more common symptoms of Mast Cell Activation Syndrome.

Mast Cell Activation Syndrome: A Primer for the Gastroenterologist
Mast Cell Activation Syndrome: A Primer for the Gastroenterologist Leonard B. Weinstock, Laura A. Pace, Ali Rezaie, Lawrence B. Afrin & Gerhard J. Molderings

Progressive Muscle Relaxation for Adults
When we experience anxiety or stress, our muscles can tense up. Progressive muscle relaxation can help to alleviate this tension and promote a sense of calm.

MCAS Testing for Healthcare Professionals
This leaflet details some of the tests used to diagnose MCAS, how to order and handle a sample and how to read the results.

MCAS Testing
This leaflet documents some of the tests that may be used to diagnose MCAS and explains how to read the results.
Become a friend
Sign up to become a Friend of Mast Cell Action so we can keep you up to date on our progress and on how to get involved in our latest campaigns and initiatives.
Donate
Mast Cell Action relies entirely on the generosity of people like you. Please make a donation now and together we can make a difference to those affected by MCAS.







